Being diagnosed with early Chronic Kidney Disease (CKD) can be scary. CKD is an irreversible progressive disease that affects 1 in 10 Canadians.
Making lifestyle and nutrition changes can help slow down the progression of CKD, but navigating nutrition changes without the support of a registered dietitian can be confusing. People often end up using outdated food lists and over restricting their diet leading to protein energy malnutrition, unintentional weight loss and frustration.
Kidneys filter the blood in your body to remove waste and extra water to make urine. The kidneys help maintain fluid and electrolyte balance by regulating fluid, sodium, potassium and phosphorus.
Reduced kidney function which can sometimes, but not always, result in kidney failure. Nutrition interventions can protect your kidney’s function early on and slow down damage.

Chantelle Greentree, RD
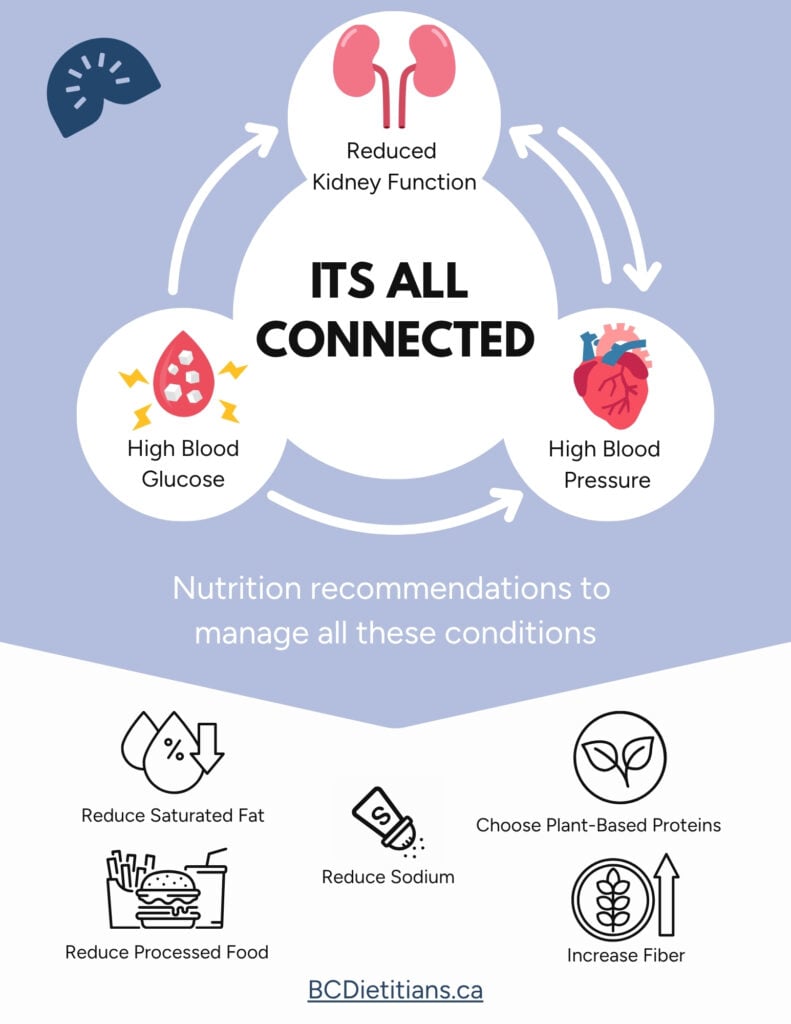
Manage Co-Morbidities: Diabetes and Hypertension
In Canada, diabetes is the leading cause of CKD, accounting for about 38%.
High blood glucose causes your kidneys to work harder to filter, increasing pressure in your kidneys. This may cause irreversible damage to your kidneys.
People with diabetes should aim to keep their blood glucose within target levels and an A1C <7.0% (blood glucose average over past 3 months) to reduce the risk of kidney damage. Learn more about managing your diabetes on our blog : What To Do Now That You’re Diagnosed With Diabetes.
The second leading cause of CKD is hypertension (high blood pressure), after diabetes.
Hypertension narrows the blood vessels in your kidneys which prevents the removal of extra fluid and waste from your body.
This leads to fluid building up in the blood vessels which increases the blood pressure and damaging your kidneys. This becomes a vicious cycle where kidney damage may cause hypertension which further damages your kidneys.
Managing both diabetes and hypertension can effectively help slow down damage to your kidneys.
Reduce sodium - the single most important change
Sodium is a mineral that is found in food and table salt (as sodium chloride). Our body uses sodium to maintain blood pressure and fluid balance as well as for muscle and nerve function.
A diet high in sodium can lead to fluid retention in the body causing increased blood pressure which can damage your kidneys and increase your risk of stroke and heart disease. Aim to reduce your daily sodium intake to <2300 mg/d.
Tips for reducing dietary sodium intake:
- Limit processed and packaged foods (ie: instant soups/noodles, chips, canned foods)
- Foods labeled with “No Added Salt” or “Low Sodium” are okay
- Flavouring alternatives eg. herbs, spices or citrus
People with CKD should always check the ingredients and avoid salt substitutes or seasonings that replace the salt with potassium additives such as “No-Salt” or “Half-Salt” as well as products labeled as “sodium-reduced“.
If you are looking for a kidney friendly salt substitute in Canada you can try Mrs. Dash which is a salt free seasoning made with spices and herbs.
Protein Recommendations for Early CKD
For early CKD, the general recommendation of 0.8 g/kg/d of protein is appropriate. For a 70kg (~150lbs) adult, this would be 50-60g of protein per day.
Protein is an important part of your daily diet to maintain and build muscle, heal and fight infections. Too little protein in your diet can lead to muscle loss.
Protein recommendations for early kidney disease stages:
- Aim for high quality animal proteins eg. fish, eggs and lean meats
- Spread protein intake throughout the day
- Avoid/limit supplemented sources like protein powders, protein gummies, protein shakes
Choose plant-based proteins (e.g., beans, lentils, seeds) more often as they are rich in fiber which can further support kidney health with:
- Better Blood Sugar Control: Fiber slows digestion which prevents blood glucose spikes after meals.
- Heart health support: Soluble fiber binds and excretes LDL (“bad” cholesterol) which can reduce risk of heart disease and high blood pressure.
- Gut Health & Decreased Inflammation: Fiber supports regular bowel movements and healthy gut bacteria which can help reduce inflammation.
- Lower Phosphorous Absorption: Phosphorus in plant foods is bound to fiber which is excreted in stool and absorbed less.
- Potassium Balance: Fiber can potentially help increase excretion of potassium in stool.

If Advised: Manage Phosphorous Intake
Phosphorus is a mineral that occurs in two forms: organic phosphorus, found naturally in foods like meats, poultry, fish, nuts, beans, and dairy products, and inorganic phosphorus, which is added to foods as a preservative or additive.
Inorganic phosphorus is commonly found in items such as dark colas, packaged foods, and deli meats. Check the ingredients list for “Phos” to find phosphorous additives in food.
Phosphorus is an important mineral for building and maintaining strong bones. Other functions of phosphorus in our body include helping us make energy and is a part of our DNA and cell structures.
Too much phosphorus causes the body to pull out calcium from your bones which will make your bones weak. The high phosphorus and calcium in your blood can increase the risk of building up in your blood vessels, lungs and heart which can lead to heart attacks, stroke or death.
In early CKD, phosphorus levels are generally not a concern as the kidneys still have sufficient function to remove excess phosphate from the body. Phosphorous management is always individualized and determined by your healthcare team based on kidney function and bloodwork.
The amount of phosphate your body absorbs depends on the source of phosphate: Organic (20-40% for plant-based and 40-60% for animal-based) vs In-Organic (90-100%).
Continue to include a variety of organic phosphate foods: fruits, vegetables, nuts, whole grains, beans, fresh meat, egg and dairy
Reduce your intake of inorganic phosphates, such as foods with added phosphorus. You can identify these by checking the ingredient list for terms that contain “phos” (eg. phosphoric acid, polyphosphate, and pyrophosphates).
If Advised: Manage Potassium Intake
Potassium is a mineral needed for our nerves to send signals so our muscles work and our heart beats regularly.
When there is too much potassium (hyperkalemia) it can lead to heart palpitations, an irregular heart beat, chest pain, shortness of breath or heart attack.
There are several non-dietary factors that can impact your serum potassium status that should be considered like common cardiovascular disease medications (ACE inhibitors, ARBs), diuretics (thiazides, lasix, spironolactone) and uncontrolled diabetes.
When blood sugar is high, potassium moves from the cells and into the blood stream causing increased potassium levels in your blood. Improving constipation can also help remove excess potassium through stool.
Potassium management is always individualized and determined by your healthcare team based on kidney function and labwork.
Here are some ways to help reduce excess potassium through diet:
- Include whole fruits and vegetables – the fiber decreases potassium absorption
- Check ingredient list for potassium additives eg. potassium lactate, potassium chloride (common salt substitute), potassium phosphate and potassium acetate
- Reduce ultra-processed foods (sodas, processed meats/cheeses, packaged snacks like cookies, chips, cakes)
- Boiling and soaking can reduce potassium amount eg. potatoes, root vegetables, beans
- Ingredient preparation can impact potassium content ie. dried fruits have higher potassium compared to fresh whole fruit
- All foods can still be enjoyed by adjusting portion sizes
Key takeaways for kidney nutrition
Nutrition interventions for early CKD should focus on maintaining a general healthy diet and managing comorbidities (diabetes, CVD and hypertension) to slow down disease progression.
- Continue to include a variety of fruits and vegetables.
- Adequate protein intake to minimize muscle loss
- Choose plant-based proteins more often.
- Reduce sodium <2300mg/d to minimize fluid retention and hypertension
- Potassium and phosphate additives in processed foods have high absorption in the body.
- Potassium and phosphorus in whole foods (fruits, vegetables, grains, fresh meats, dairy products etc) are less absorbed in the body and are part of a healthy diet.
For more individualized nutrition advice, speak with a renal dietitian for kidney health. A renal dietitian is someone who specialize in kidney diseases and can help you determine the appropriate diet for your kidney health.
References:
Alberta Health Services. (n.d.). Nutrition guidelines for chronic kidney disease [PDF]. https://www.albertahealthservices.ca/assets/info/nutrition/if-nfs-ng-renal.pdf
Alberta Health Services. (n.d.). Chronic kidney disease: Care instructions. https://myhealth.alberta.ca/Health/aftercareinformation/pages/conditions.aspx?hwid=ud1309
BC Renal. (2024). Healthy eating for your kidneys [PDF]. https://www.bcrenal.ca/resource-gallery/Documents/Healthy_Eating_For_Your_Kidneys.pdf
Health Canada. (2022, June 30). Sodium. Government of Canada. https://www.canada.ca/en/health-canada/services/nutrients/sodium.html
Kitzler, T. M., & Chun, J. (2023). Understanding the Current Landscape of Kidney Disease in Canada to Advance Precision Medicine Guided Personalized Care. Canadian journal of kidney health and disease, 10, 20543581231154185. https://doi.org/10.1177/20543581231154185
National Institute of Diabetes and Digestive and Kidney Diseases. (2025). Healthy eating for adults with chronic kidney disease. https://www.niddk.nih.gov/health-information/kidney-disease/chronic-kidney-disease-ckd/healthy-eating-adults-chronic-kidney-disease
The Kidney Foundation of Canada. (2020). Chronic kidney disease [PDF]. https://kidney.ca/CMSPages/GetFile.aspx?guid=9a5bb7de-9cf3-4859-ac39-a9f57429d900
National Kidney Foundation. (2024, July 16). Phosphorus and your CKD diet. https://www.kidney.org/kidney-topics/phosphorus-and-your-ckd-diet
National Kidney Foundation. (2023, February 1). Potassium. https://www.kidney.org/kidney-topics/potassium
National Kidney Foundation. (n.d.). CKD diet: How much protein is the right amount? https://www.kidney.org/kidney-topics/ckd-diet-how-much-protein-right-amount
National Kidney Foundation. (2022). Kidney disease and protein [PDF]. https://www.kidney.org/sites/default/files/kidney-disease-and-protein-english.pdf
National Kidney Foundation. (n.d.). High blood pressure and chronic kidney disease. https://www.kidney.org/high-blood-pressure-and-chronic-kidney-disease






Add a comment